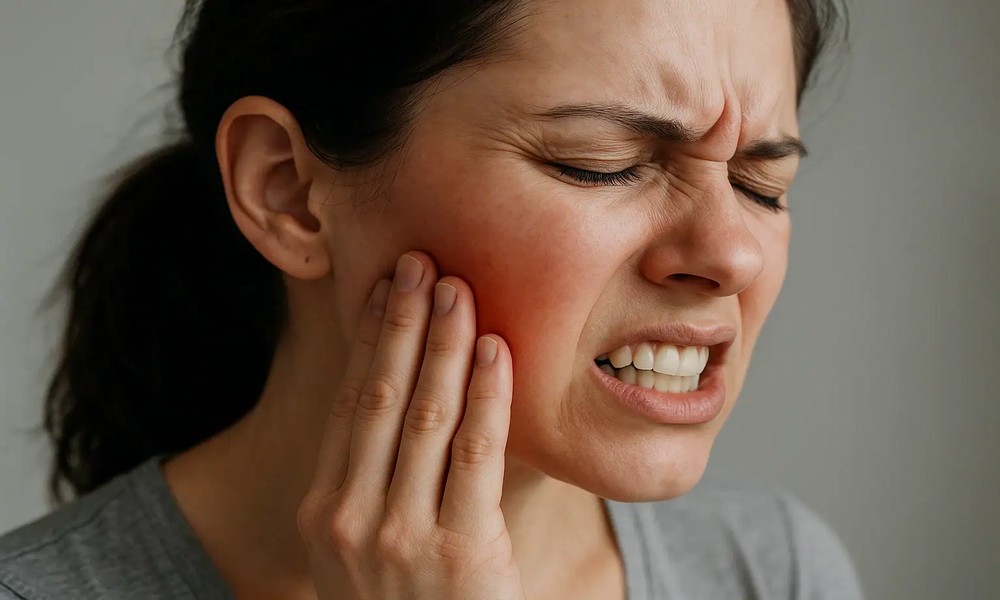
Waking up with a sore jaw, a dull headache behind your eyes, or teeth that feel like they’ve been through a workout all night is more common than most people think. A lot of adults in Burley and across the Magic Valley live with it for years, assuming it’s just stress or a bad pillow. The actual cause is usually more specific, and in a real percentage of cases, it’s pointing to something bigger than the jaw itself. At All Smiles Dental, Dr. Spencer Rice works with patients every week who arrive convinced they just need a night guard and leave with a much clearer picture of what’s actually happening while they sleep.
Here’s what the morning jaw ache usually means, how a proper diagnosis works, and why the treatment depends entirely on what’s driving the grinding in the first place.
The Three Conditions That Usually Overlap
Bruxism, TMJ disorder, and sleep apnea get discussed as separate problems, but in real patients they tend to run together. Understanding how they interact is the starting point for figuring out what’s wrong.
Bruxism is the clinical term for clenching and grinding. It can happen during the day as a stress response, or at night as a sleep-related movement disorder. Nighttime bruxism is the more destructive version because you can’t consciously control it and because the forces involved are significantly higher than anything you’d generate while awake.
TMJ disorder, or more accurately temporomandibular joint dysfunction, refers to problems with the joint that connects your lower jaw to your skull. Symptoms include jaw pain, clicking or popping, limited opening, ear fullness, and headaches concentrated around the temples. TMJ problems can cause bruxism, and chronic bruxism can cause TMJ problems. The cause-and-effect relationship runs both directions.
Sleep apnea is the third piece, and it’s the one most patients don’t expect. When the airway partially collapses during sleep, the body often responds by clenching the jaw and thrusting it forward to reopen the airway. That protective reflex, repeated hundreds of times a night, produces exactly the symptoms of bruxism. Treating the grinding without addressing the underlying apnea is like treating a cough without addressing the infection.
The Symptoms That Point to Each
Patients who come in describing morning jaw pain usually have one or more of the following:
- Teeth that are visibly worn flat, chipped, or shorter than they used to be
- Sensitivity to cold or pressure, especially on back teeth
- Headaches that are worst in the morning and ease through the day
- Ear pain, ringing, or a feeling of fullness that isn’t from an ear infection
- A jaw that clicks, pops, or catches when opening and closing
- Pain when chewing tough foods
- A partner who reports grinding sounds at night
- Daytime fatigue despite sleeping a full night
The combination matters. Morning headaches plus daytime fatigue plus grinding strongly suggests sleep-disordered breathing. Jaw clicking plus chewing pain plus limited opening suggests a primary TMJ issue. Visible tooth wear with no other symptoms is often straightforward bruxism related to stress or bite issues.
How Dr. Rice Actually Diagnoses the Root Cause
The diagnostic process at All Smiles Dental goes beyond a quick look at your teeth. Several tools and exam steps work together to identify what’s actually driving the symptoms.
Cone beam CT imaging captures a three-dimensional view of the jaw joints, the airway, and the supporting bone. Unlike traditional dental X-rays, cone beam imaging shows the condyle of the jaw joint, the position of the disc, and the shape and dimensions of the upper airway. Airway narrowing visible on cone beam scans is often the first clue that a grinding problem has a sleep apnea component.
Occlusal analysis examines how your teeth actually come together. Small imbalances in the bite, called occlusal interferences, can trigger protective muscle patterns that show up as clenching and grinding. Digital occlusal analysis tools can measure where the bite forces are concentrated and whether certain teeth are taking more load than they should.
Clinical examination of the jaw muscles, the joint itself, and the range of motion fills in the picture. Tender muscles, limited opening, or joint sounds all point toward specific diagnoses.
Patient history matters as much as the imaging. Questions about sleep quality, snoring, witnessed apneas, daytime energy, and stress levels often change the direction of the workup. When sleep-disordered breathing is suspected, a referral for a formal sleep study is the next step. The American Academy of Sleep Medicine sets the diagnostic standards for sleep apnea, and a dental exam alone cannot confirm or rule it out.
Why Over-the-Counter Night Guards Often Make Things Worse
The drugstore night guard is a common first step for patients trying to handle the problem cheaply. It sometimes helps. It also sometimes makes things significantly worse, and the reasons are worth understanding.
Over-the-counter night guards have several real problems:
- They don’t fit the specific shape of your teeth, so they shift during the night and can reposition the jaw in ways that stress the joint
- They’re usually made of soft material, which some patients chew against more aggressively than they would chew against their own teeth
- They provide no bite adjustment, meaning the underlying occlusal issues driving the grinding are unaddressed
- They cover either the top or bottom arch fully, which in sleep apnea cases can worsen airway collapse
A custom-fitted appliance from a dentist takes specific measurements, addresses the bite relationship, and is fabricated from materials chosen for the patient’s specific situation. Some patients need a simple protective guard. Others need a mandibular advancement device that both protects the teeth and opens the airway during sleep. The right appliance depends entirely on the diagnosis.
When Grinding Points to Something Bigger
The patients who benefit most from a thorough workup are the ones whose grinding is a symptom of undiagnosed sleep apnea. Treating the grinding without addressing the apnea leaves the more serious condition in place, and sleep apnea has real cardiovascular and metabolic consequences over time.
Red flags that suggest a sleep study is warranted:
- Loud snoring, particularly if it stops and starts
- A bed partner who has noticed breathing pauses
- Morning headaches or dry mouth on waking
- Daytime sleepiness that isn’t explained by short sleep
- High blood pressure that’s difficult to control
- Weight gain concentrated around the neck and chest
A dental appointment is often where these connections first get made, because dentists see the mouth and airway in ways that general physicians typically don’t. The American Dental Association’s guidance on dental sleep medicine has expanded significantly over the past decade, and many patients are diagnosed with sleep apnea because a dentist recognized the pattern during a routine exam.
Getting a Real Answer Instead of Just a Mouthpiece
Morning jaw pain is a symptom, not a diagnosis. The right response depends on finding out what’s actually causing it, and that takes more than a quick look and a generic appliance.
If you’ve been waking up with jaw pain, headaches, or worn teeth and you want a real answer, contact All Smiles Dental in Burley to schedule an evaluation with Dr. Rice. A thorough workup produces a treatment plan that fits your specific situation, and often reveals connections that weren’t obvious from the symptoms alone.